Post-Op Dental Implant Instructions: A Comprehensive Guide
Following dental implant surgery, diligent aftercare is paramount for successful osseointegration and long-term implant health, ensuring both function and aesthetics.
Immediate Post-Operative Care (First 24-48 Hours)
The initial 24-48 hours are critical for proper healing. Immediately post-surgery, apply firm, consistent pressure to the surgical site with gauze pads provided by your dentist for at least 30-60 minutes, or until bleeding subsides. Avoid rinsing vigorously, spitting, or using straws, as these can dislodge the blood clot essential for healing.
Rest is paramount; limit physical activity. Ice packs applied to the cheek in 20-minute intervals (20 minutes on, 20 minutes off) will minimize swelling and discomfort. Stick to a liquid diet – water, broth, and clear juices are ideal. Avoid hot foods and beverages.
Take prescribed medications as directed, including pain relievers and antibiotics. Report any excessive bleeding, severe pain not relieved by medication, or signs of infection (fever, pus) to your dentist immediately. Gentle care during this phase sets the stage for successful implant integration.
Bleeding Management
Some bleeding is normal following dental implant surgery, but excessive bleeding requires attention. Immediately after the procedure, bite down firmly on the gauze pads provided for 30-60 minutes, maintaining consistent pressure. If bleeding persists, replace the gauze with fresh pads every 30 minutes until it slows.
Avoid disturbing the surgical site. Do not rinse vigorously, spit, or use straws for the first 24 hours, as these actions can dislodge the forming blood clot. A small amount of pink-tinged saliva is normal.
If bleeding continues unabated, apply a moistened tea bag (black tea contains tannic acid, which aids clotting) to the site, biting down gently. Contact your dentist immediately if bleeding is profuse or doesn’t respond to these measures. Maintaining clot stability is crucial for optimal healing and preventing complications.
Pain Control & Medication
Post-operative discomfort is expected after dental implant surgery, but can be effectively managed. Your dentist will likely prescribe pain medication – take it as directed, even if you feel minimal pain, to stay ahead of discomfort. Over-the-counter pain relievers, like ibuprofen or acetaminophen, may also be recommended or used in conjunction with prescription medication;

Avoid exceeding the recommended dosage of any medication. If you experience persistent or severe pain despite medication, contact your dentist. Applying ice packs to the outside of your cheek in 20-minute intervals can also help reduce pain and swelling.
Remember to inform your dentist of any allergies or medical conditions before taking any medication. Proper pain management is vital for a comfortable recovery and adherence to post-operative instructions.
Swelling & Bruising Management
Swelling and bruising are common after dental implant surgery, peaking typically within 24-72 hours. Applying ice packs to the outside of your face for 20 minutes on, 20 minutes off, during the first 48-72 hours is crucial. Elevating your head with extra pillows, even while sleeping, also minimizes swelling.
After 72 hours, switch to warm compresses to encourage blood flow and reduce bruising. While bruising may appear, it usually resolves within a week or two. Avoid strenuous activity, as it can exacerbate swelling.
If swelling or bruising significantly increases after the first few days, or if you notice signs of infection (fever, increased pain, pus), contact your dentist immediately. Gentle care and following these guidelines will help manage these common post-operative effects.
Dietary Restrictions: Initial Phase
Following your dental implant surgery, adhering to a soft food diet is essential for optimal healing and to avoid disrupting the surgical site. For the first 24-48 hours, consume only liquids like broth, smoothies (without seeds), and yogurt. Gradually introduce soft foods such as mashed potatoes, applesauce, scrambled eggs, and well-cooked pasta.
Avoid hard, crunchy, chewy, or spicy foods that could irritate the area or put stress on the implant. Also, refrain from extremely hot or cold temperatures. Ensure all foods are easy to chew and swallow.
As healing progresses, you can slowly reintroduce more solid foods, but continue to avoid anything that causes discomfort. Maintaining proper nutrition supports the healing process, so prioritize nutrient-rich, soft options.
Oral Hygiene: Gentle Cleaning
Maintaining excellent oral hygiene is crucial, even immediately after implant surgery, but requires a gentle approach. For the first few days, avoid brushing directly on or near the implant site. Instead, gently rinse your mouth with a warm saltwater solution (1/2 teaspoon salt in 8 ounces of water) several times a day, especially after meals.
After 24-48 hours, you can begin gently brushing your teeth, carefully avoiding the surgical area. Use a soft-bristled toothbrush and avoid vigorous scrubbing. Your dentist may recommend a special antimicrobial mouthwash to help prevent infection.
Continue this gentle cleaning routine until your dentist approves a return to your normal oral hygiene practices. Proper hygiene minimizes the risk of complications and promotes healing.
Long-Term Care & Maintenance
Ensuring the longevity of your dental implant requires a commitment to long-term care and maintenance, mirroring the care you give your natural teeth. Regular dental check-ups – typically every six months – are essential for monitoring the implant’s stability and the health of the surrounding gum tissues.
Professional cleanings are vital to remove plaque and tartar buildup, preventing peri-implantitis, an inflammation around the implant. Maintaining excellent at-home oral hygiene, including gentle brushing and flossing, is equally important.
Be proactive in reporting any changes, such as increased pain, swelling, or mobility, to your dentist promptly. Lifestyle factors, like avoiding smoking, also contribute to implant success. Consistent care safeguards your investment and smile for years to come.
Gentle Brushing Techniques Around the Implant
After dental implant placement, adopting a gentle brushing technique is crucial to avoid disrupting the healing process and protect the implant site. Use a soft-bristled toothbrush and avoid vigorous scrubbing, which can irritate the gums.
Focus on cleaning along the gumline, ensuring you remove plaque and food particles without applying excessive pressure. Angle the brush at a 45-degree angle towards the gumline, using small, circular motions. Pay attention to all surfaces of the teeth and the implant crown.
Initially, gentle brushing may be sufficient; as healing progresses, you can gradually increase the pressure. Consider using an interdental brush to clean between teeth and around the implant. Consistent, gentle brushing is key to maintaining optimal oral hygiene.
Flossing & Interdental Cleaning
Maintaining cleanliness between teeth and around the implant is vital for preventing peri-implantitis and ensuring long-term success. Traditional flossing can be tricky around implants; consider using floss threaders or specialized interdental brushes.
Interdental brushes, available in various sizes, effectively remove plaque and debris from between teeth and around the implant abutment. Gently insert the brush between teeth, using a back-and-forth motion. Avoid forcing the brush, as this could damage the gums.
Water flossers can also be beneficial, providing a gentle stream of water to dislodge food particles. Regular interdental cleaning, alongside brushing, is essential for maintaining optimal oral hygiene and preventing inflammation. Consult your dentist for personalized recommendations.
Regular Dental Check-ups & Professional Cleanings
Consistent professional dental care is non-negotiable for the longevity of your dental implant. Schedule regular check-ups – typically every six months – even if you experience no apparent issues. These appointments allow your dentist to monitor the implant’s stability and surrounding gum tissue.
Professional cleanings remove hardened plaque (tartar) that brushing and flossing miss, preventing peri-implantitis. Your hygienist will use specialized instruments designed to clean around implants without causing damage. Early detection of any problems is crucial.
During check-ups, your dentist will assess your bite, ensuring it’s not placing undue stress on the implant. They’ll also evaluate the health of your gums and surrounding bone. Adhering to a schedule of regular visits safeguards your investment and oral health.
Recognizing & Addressing Potential Complications
While dental implant surgery boasts a high success rate, being aware of potential complications is vital for prompt intervention. Implant failure, though rare, can occur, manifesting as mobility or increasing pain. Early detection significantly improves treatment outcomes.
Signs of infection – fever, escalating pain, visible pus, or swelling – demand immediate attention. Contact your dentist immediately; untreated infections can jeopardize the implant. Peri-implantitis, gum inflammation around the implant, is another concern. Symptoms include redness, bleeding, and potential bone loss.
Don’t ignore persistent discomfort or changes in your bite. Promptly report any unusual sensations to your dental team. Addressing complications swiftly minimizes long-term issues and preserves your oral health investment. Ignoring symptoms can lead to more extensive and costly treatments.
Signs of Infection (Fever, Increased Pain, Pus)
Post-implant surgery, vigilance for infection is crucial. A fever exceeding 100.4°F (38°C) is a significant warning sign, indicating your body is fighting an infection. Increased pain, disproportionate to the expected post-operative discomfort, should also raise concern. Pain that intensifies days after surgery, rather than subsiding, warrants immediate attention.
The presence of pus – a thick, yellowish or greenish discharge – around the implant site is a clear indicator of infection. Visible swelling, redness, and warmth surrounding the area are also red flags. Any foul odor emanating from the surgical site is equally concerning.
Contact your oral surgeon immediately if you experience any of these symptoms. Untreated infections can lead to implant failure and systemic health issues. Do not attempt self-treatment; professional intervention is essential.
Implant Failure Symptoms
While rare, implant failure can occur. Recognizing the symptoms early is vital for potential intervention. Persistent pain around the implant, despite medication, is a key indicator. Increased mobility of the implant, or a feeling that it’s “loose,” suggests a lack of osseointegration – the crucial bone fusion process.
Swelling and inflammation that don’t subside within a reasonable timeframe, or that return after initially improving, can signal failure. Bleeding around the implant site, especially if it’s spontaneous, is also concerning. Difficulty chewing or a change in your bite alignment may also occur.
Promptly contact your oral surgeon if you experience any of these symptoms. Early detection increases the chances of successful treatment, which may involve revision surgery or alternative solutions. Ignoring these signs can lead to further complications.
Managing Peri-Implantitis (Gum Inflammation)
Peri-implantitis, inflammation around the implant, requires proactive management. It’s often caused by bacterial infection, similar to gum disease. Initial signs include redness, swelling, and bleeding around the implant. Left untreated, it can lead to bone loss and, ultimately, implant failure.
Maintaining meticulous oral hygiene is crucial. This includes gentle brushing, flossing around the implant, and using recommended interdental cleaning tools. Regular professional cleanings with your dentist or periodontist are essential to remove plaque and calculus buildup.
Your dentist may recommend antimicrobial mouth rinses or localized antibiotic therapy to control the infection. In advanced cases, surgical intervention, such as debridement (cleaning the implant surface), may be necessary. Early detection and consistent care are key to preventing progression.
Specific Instructions for Different Implant Types
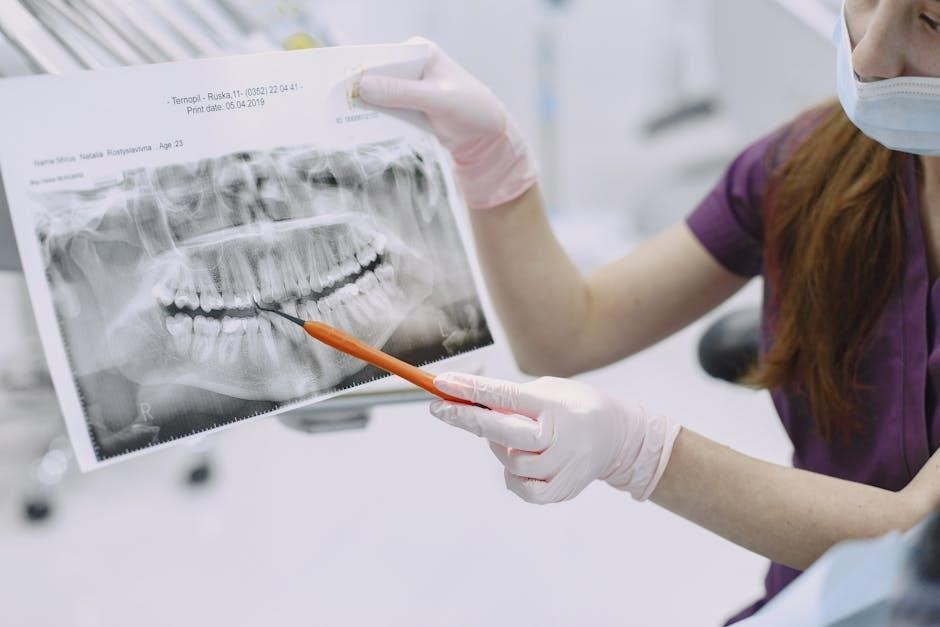
Post-operative care varies slightly depending on the implant type. Single tooth implants generally require focused care around the surgical site, emphasizing gentle cleaning and avoiding excessive force during chewing. Implant-supported bridges necessitate meticulous hygiene not only at the implant site but also along the bridge itself, requiring special floss or interdental brushes.
For implant-supported dentures, a more comprehensive cleaning routine is vital, including removing the denture for cleaning and thoroughly brushing both the denture and the underlying implants. Pay close attention to areas where the denture contacts the gums.
Always follow your dentist’s specific instructions, as they are tailored to your individual case and the implant system used. Consistent adherence to these guidelines maximizes the chances of successful integration and long-term stability.
Instructions for Single Tooth Implants
Following placement of a single tooth implant, prioritize gentle care. For the initial 24-48 hours, strictly adhere to a soft food diet, avoiding chewing directly on the implant site. Maintain meticulous oral hygiene, gently rinsing with saltwater after meals to dislodge debris. Avoid vigorous brushing near the implant; instead, use a soft-bristled brush and gentle circular motions.
Monitor for swelling and bleeding, applying ice packs intermittently to reduce discomfort. Take prescribed pain medication as directed. Avoid smoking and strenuous activity, as these can impede healing.
Gradually reintroduce firmer foods as comfort allows, and continue diligent oral hygiene practices. Regular dental check-ups are crucial to monitor implant integration and long-term health.
Instructions for Implant-Supported Bridges
Post-operative care for implant-supported bridges requires extra diligence. Initially, a soft diet is essential, avoiding any force on the bridge while osseointegration occurs. Gentle rinsing with saltwater after each meal is vital to keep the area clean, but avoid disturbing the surgical site.
Pay close attention to hygiene around the bridge and implants. Use interdental brushes or floss threaders to clean beneath the bridge where it meets the gums. Monitor for any signs of inflammation or loosening.
Regular dental visits are paramount to assess the bridge’s fit, stability, and the health of the surrounding tissues. Avoid parafunctional habits like clenching or grinding, which can compromise the implants. Proper maintenance ensures longevity and optimal function.
Instructions for Implant-Supported Dentures
Implant-supported dentures demand meticulous post-operative care. Begin with a soft food diet, gradually reintroducing firmer foods as healing progresses and the implants integrate. Avoid placing excessive pressure on the denture during the initial healing phase.
Daily removal of the denture for cleaning is crucial. Gently brush the denture with a soft-bristled brush and denture cleaner, avoiding abrasive pastes. Simultaneously, clean the implant abutments and surrounding gum tissues with a separate soft brush.
Regular dental check-ups are essential to evaluate the fit, stability, and hygiene of both the denture and implants. Address any discomfort or signs of irritation promptly. Proper care minimizes complications and maximizes the denture’s function and longevity.
Lifestyle Adjustments for Optimal Healing
Post-implant placement necessitates temporary lifestyle modifications to promote optimal healing. Refrain from smoking, as it significantly impairs blood flow and delays osseointegration, increasing the risk of implant failure. Limit strenuous physical activity for at least 72 hours, avoiding any activity that could increase blood pressure.
Prioritize adequate rest and hydration. A well-rested body heals more efficiently. Drink plenty of water to maintain oral moisture and support tissue repair. Avoid touching the surgical site with your tongue or fingers to prevent infection.
Minimize sun exposure to the surgical area, as it can contribute to swelling. Consider stress-reducing activities, as stress can negatively impact the immune system and healing process. Following these adjustments will contribute to a smoother recovery.